I first noticed it in February; in the awful week of illness, following my lumbar puncture. Whilst battling sickness and headaches and strange sensations whenever I stood up, I also realised that my oxygen saturations were a little low. My body wasn’t getting enough O2.
Since becoming an oxygen user in 2016, the amount of O2 I need, hasn’t changed. Normally, Pulmonary Venous Occlusive Disease (PVOD) is characterised by a rapid decline in lung function, and thus a rapid need for more and more medicinal oxygen. But thankfully, so far, I’ve miraculously avoided this fate. For the past six years, if I’m sitting down or resting or not doing any activity, my lungs can happily oxygenate my body on room air, and my oxygen saturation level is usually 97%. Completely normal 🙂 And even better, in recent years, when I’m quickly sneaking to the loo or kitchen, my saturations remain high, without any need for O2 either. 🙂 However with longer or harder activities -like climbing the stairs, hanging up the washing, or playing tug with Kepler- I need some extra help. Four litres of lovely, cool oxygen per minute, through my noisy concentrator machine or heavy portable cylinders, and my saturations remain in the normal range, and thus my body happy. 😀 They occasionally fall lower when my body is fighting an illness; but for the majority -sometimes with oxygen, sometimes without- my levels are 97%. Always. And that is how it has been for the past six years. Constant, consistent, stable. 🙂 Until now.

My lungs are currently struggling, and we don’t know why. For at least seven weeks, my body has been finding it difficult to keep adequately oxygenated. Even when breathing in lovely oxygen, my saturation levels are much lower than is safe. When sitting down on room air, they hover around the low nineties. When nipping to the loo on room air, they plummet to the eighties. And if I try to do housework or walk about -whilst wearing my oxygen- they plummet to the low eighties, or occasionally even the seventies. Yep, they’re falling to dangerously low levels, even when I’m breathing in O2! But the strangest part is I feel fine. Absolutely fine. In the past, low oxygen saturations have made me feel ill. Sick and weak and fatigued. But not currently. Sometimes I feel more breathless than usual, but there’s none of the other debilitating symptoms. In fact, I’m doing more this Winter and Spring than ever before. Walking the dogs and climbing the stairs multiple times a day and even cleaning the house! These are all new achievements! And I feel good… until I get out my pulse oximeter. And stranger still, it is not consistent. Most of the time they’re falling, but sometimes they just behave normally. Like when a doctor is watching! 😉 Something is not right.
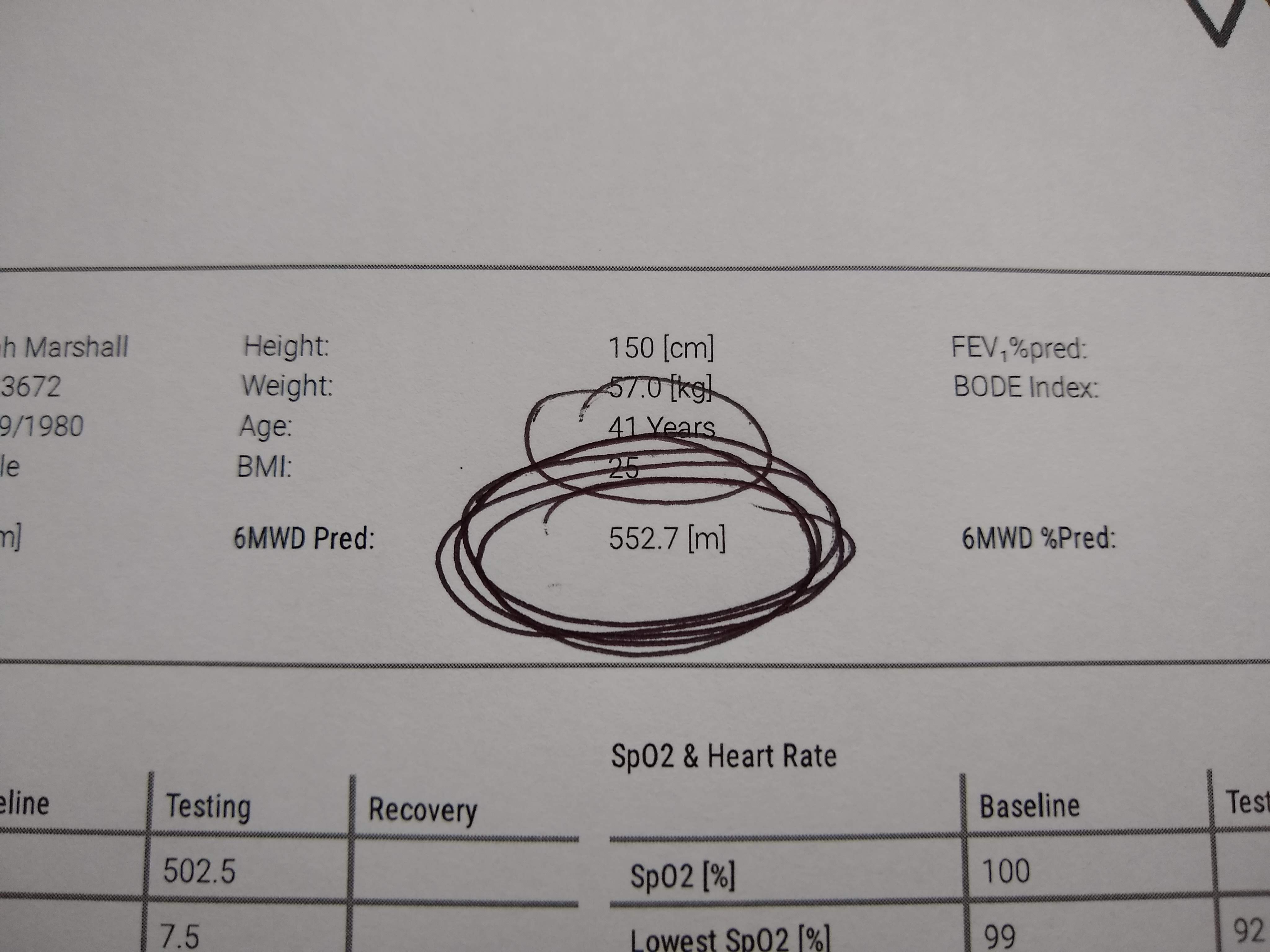
At first, I monitored, monitored, monitored. But with no improvement after a month, my PH and transplant teams both started the tests. I’d had a full PH check-up only weeks earlier (the day before the lumbar puncture). I’d walked 460m on the six minute walk test (carrying my heavy cylinders myself), my bloods were fine, and the echocardiogram looked like a normal person’s heart. All good news. But despite that reassurance, we repeated them all twice, plus urine tests, a chest X-ray and CT scan. A thorough MOT. Happily everything looks normal. No change from the month earlier, and no change compared to last year. And to demonstrate my current strange inconsistencies- I managed 400m in one 6MWT and 552m in the other! The latter, not only a personal best, but a Harefield pre-transplant patient best! Wahoo! But although I’m pleased and thankful that everything looks hunkey-dory, and there’s no obvious problem; it does, once again, leave questions and confusion. And thus no solution.









Maybe my body is fighting an infection that is taking longer than normal to shift. I do have raised white blood cells, but the other infection markers are normal. Maybe the lumbar puncture did some unknown damage. I noticed it afterwards, but it could have started earlier, and there’s no logical connection. Maybe I’ve got blood clots from stopping the warfarin. We couldn’t find any, but not all clots are observable. Maybe I’m deteriorating. I’m long overdue my PVOD decline, but my pulmonary pressures and lungs look unchanged. Maybe it’s just a winter blip. We just don’t know.
So for now I am waiting and watching and hoping and praying. I’ve upped my oxygen to five litres, am wearing a full face mask to ensure inhalation (I’m a mouth breather) and am keeping active. But even with these changes, my oxygen saturations are still behaving unusually. Harefield are ready to ‘un-pause’ me on the active transplant list if it continues; but I have all my fingers crossed it will right itself before then.



Thankfully as I feel well, I’m still happy and busy and able to enjoy life. But there is a nagging fear, that a decline or transplant could happen just as we’re moving house and embarking on a new adventure. I developed PH six months after moving into our current home, and it made it difficult to integrate ourselves into the community and refurbish the house. I really, really, really don’t want that to happen again. I’m praying that I stay healthy and well, so we can have the Peak District adventures, that we’re so excited for.
Come on wonderful lungs! 🙂
I have enjoyed reading your blog and love your optimistic attitude. I was originally diagnosed with PVOD – was on transplant list, but like you, I was doing exceptionally well. No oxygen needed at rest and saturation levels dropped during activity. Then a PH pulmonologist suggested a lung biopsy. The results were very telling – I did not have PVOD but rather HP (hypersensitivity pneumonitis). This made more sense and explained the drop in oxygen upon movement. It’s an inflammation in the lungs. Doctors feel the HP is what led to my PH. Like you we also moved as there was something causing the HP but we could not identify it. My CT scans showed great improvement following the move and I’m hopeful that I will continue to heal. Prayers for you – I could not believe the ordeal you endured in February but, at least for me, it takes a long time to bounce back from illness. Hopefully that’s what is going on with you.
Blessings to you.
LikeLike